Breast Reconstruction
In Tucson, AZ


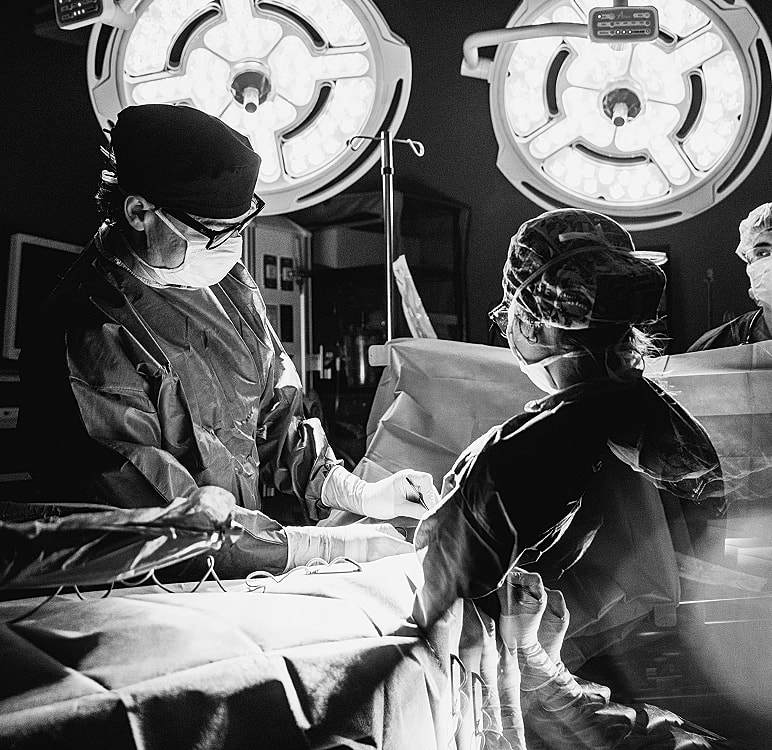
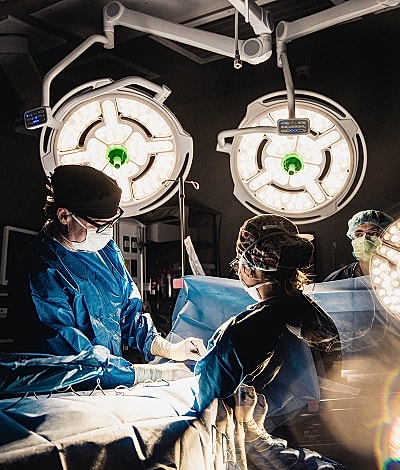
Breast reconstruction is an important step for many women after breast cancer treatment, mastectomy, or breast reduction surgery. Reconstruction surgery helps restore a natural breast mound, balance the body, and provide a sense of wholeness during recovery.
Dr. James offers a full spectrum of breast reconstruction techniques, from implant reconstruction to advanced flap reconstruction using your own autologous tissue. As a board-certified plastic surgeon with fellowship training in microsurgery at UCLA, Dr. James brings precision, artistry, and compassion to every procedure.

Breast reconstruction surgery is a form of plastic and reconstructive surgery that rebuilds the breast after breast cancer surgery, breast tissue removal, or trauma. The goal is to recreate a breast mound that looks natural and feels balanced with the other breast. Dr. James helps each patient understand the safest and most effective timing for their reconstructive surgery.


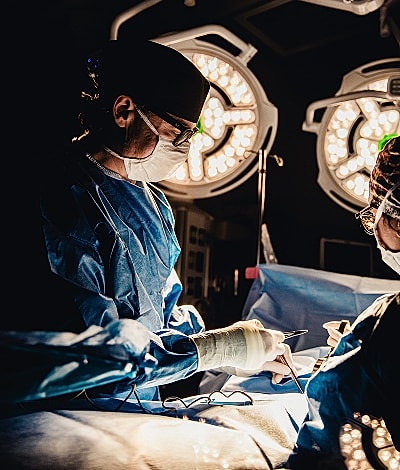
Your reconstruction surgery begins with a consultation where Dr. James reviews your breast cancer diagnosis, treatment history, and personal goals. He will explain the types of breast reconstruction available, from implant-based methods to flap surgery, and help you decide which is right for you. Depending on your chosen breast reconstruction method, surgery may take several hours. For flap procedures, microsurgery is used to reattach blood vessels and restore blood supply to the transferred tissue. Dr. James’s specialized microsurgical training ensures precision and improved outcomes for complex flap reconstruction.
Common breast reconstruction options include:
Breast reconstructive surgery is commonly performed for:

Every patient’s journey is unique, and Dr. James tailors each breast reconstruction surgery to meet those personal needs.
As such, the benefits of breast reconstruction are physical, emotional, and deeply personal. They include:
Most women who undergo breast cancer surgery are candidates for breast reconstructive surgery. Ideal candidates are healthy enough for invasive surgery and have completed, or are planning, cancer treatment such as chemotherapy and radiation therapy.
Some flap procedures, such as the DIEP flap or TRAM flap, require enough fatty tissue in the lower abdomen for transfer. Others, like the PAP flap or TUG flap, may use tissue from the upper inner thigh. Implant reconstruction is an option for women who prefer less invasive surgery or do not have enough donor tissue. Dr. James carefully evaluates each patient to recommend the safest and most effective breast reconstruction method for her body type.

Recovery depends on the type of procedure. Implant reconstruction with tissue expanders and silicone implants generally allows for a shorter recovery time. Flap reconstruction, such as DIEP flap or latissimus dorsi flap, usually involves a longer recovery due to abdominal surgery or tissue transfer.
Patients may need to avoid heavy lifting and strenuous exercise for several weeks. Scar tissue and healing vary, but most women are able to return to everyday life within a few months. Dr. James provides ongoing follow-up and guides patients through recovery with compassion and attentiveness.

The goal of breast reconstructive surgery is to restore a natural breast appearance that feels balanced and comfortable.
For patients who undergo autologous breast reconstruction, results often last a lifetime since the tissue ages with the body like a natural breast. Implant reconstruction may require revision over time if there is implant rupture or changes in breast shape.
Additional procedures such as nipple reconstruction, fat grafting, or breast lift may be performed later to refine the reconstructed breast.
Dr. James Rough is a board-certified plastic surgeon with advanced fellowship training in microsurgery. His expertise in complex flap procedures, such as the DIEP flap and TRAM flap, allows him to offer breast reconstruction patients the most advanced reconstructive surgery available.
Beyond his technical skill, patients trust Dr. James for his compassionate approach and commitment to patient-centered care. He takes the time to explain breast reconstruction options clearly, listen to concerns, and ensure each patient feels supported throughout their journey.
Yes. According to the Women’s Health and Cancer Rights Act, insurance providers must cover breast reconstruction after mastectomy, including surgery on the other breast for symmetry.
Immediate reconstruction is performed during the same surgery as mastectomy, while delayed reconstruction happens months or years later after cancer treatment is complete.
Like all invasive surgeries, risks include infection, scar tissue, implant rupture, or issues with blood supply in flap procedures. Dr. James will discuss these with you during your consultation.
The deep inferior epigastric perforator (DIEP) flap is a type of free flap reconstruction where the surgeon takes tissue from the lower abdomen, reattaches blood vessels to the chest wall, and forms a new breast without sacrificing abdominal muscle.
Yes. Nipple reconstruction and tattooing are options once the reconstructed breast has healed, restoring the appearance of the nipple and areola.
Radiation therapy can affect breast skin and scar tissue. Some women may delay reconstruction or choose specific techniques to minimize risks.
Other types of flap surgery include the TRAM flap, SIEA flap, PAP flap, TUG flap, and latissimus dorsi flap. Each uses a different donor site, such as the abdomen, upper thigh, or back.
No. Breast reconstruction does not prevent breast cancer. Regular breast cancer screening remains important even after reconstructive surgery.